

NEMT Entrepreneur provides expert insights, strategies, and resources to help non-emergency medical transportation professionals grow their businesses. Get industry-leading advice to succeed in NEMT.
Featured articles
When it comes to pricing for non-emergency medical transportation (NEMT), providers typically choose between flat-rate pricing or mileage-based pricing - or a combination of both. Each model has its strengths and drawbacks, depending on factors like trip distances, service levels, and administrative requirements. Here's a quick breakdown:
- Flat-rate pricing: Charges a fixed fee per trip, making it predictable and easy to manage. Best suited for short, consistent routes in urban areas or facility contracts. However, it may lead to losses on longer trips.
- Mileage-based pricing: Combines a base fee with per-mile charges, offering flexibility for varied distances. Ideal for rural markets or trips with unpredictable lengths. It requires more detailed documentation and accurate mileage tracking.
- Hybrid models: Blend both approaches, using a base rate plus mileage for longer trips. This method balances cost recovery and transparency, especially for Medicaid contracts or mixed payer types.
Each pricing structure impacts profitability, customer satisfaction, and compliance. Understanding your market and trip patterns is key to selecting the best option. Below is a comparison to help you decide.
Quick Comparison
| Feature | Flat-Rate Pricing | Mileage-Based Pricing | Hybrid Pricing |
|---|---|---|---|
| Best For | Short, predictable trips | Long or variable distances | Mixed trip lengths |
| Cost Recovery | Fixed costs only | Fixed + variable costs | Balanced |
| Administrative Effort | Low | High | Moderate |
| Transparency | Simple for clients | Detailed breakdown | Combines both |
The right pricing model depends on your service area, trip variability, and client base. Keep reading for an in-depth look at these pricing strategies and how to implement them effectively.
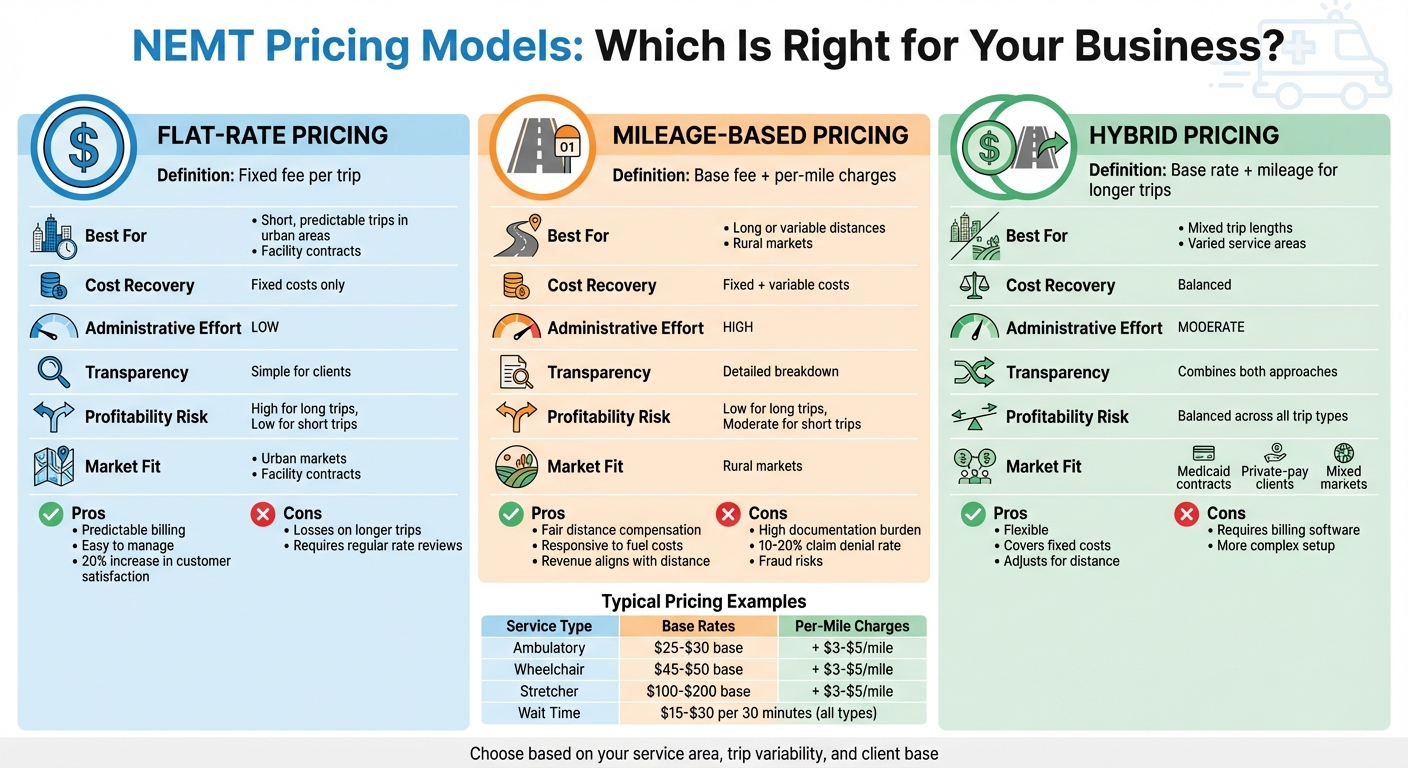
NEMT Pricing Models Comparison: Flat-Rate vs Mileage-Based vs Hybrid
How to Set Prices for NEMT: Increase Private Pay Clients with These 3 Tips
Core Elements of NEMT Pricing
To run a profitable Non-Emergency Medical Transportation (NEMT) business, you need a solid grasp of the costs involved. Every pricing decision hinges on understanding your expenses and the factors that shape the true cost of each trip.
Fixed and Variable Costs
Fixed costs stay the same no matter how many trips you complete. These include expenses like vehicle leases or loans, insurance, software subscriptions for dispatch and billing, licensing, permits, and base administrative salaries.
On the other hand, variable costs change with the level of business activity. Fuel, maintenance, and driver wages all increase as trip volume grows. Adding more vehicles to your fleet also raises insurance premiums.
Balancing these fixed and variable costs is key to profitability. iSi Technology highlights how NEMT management software can improve operational efficiency by 20% to 40%. For example, better route optimization can cut fuel use and vehicle wear-and-tear, potentially increasing a single vehicle's annual revenue from $40,000 to $60,000.
Trip-Specific Factors
Each trip comes with its own set of variables that affect pricing. Distance is an obvious one - longer trips mean more fuel and driver time. But deadhead miles, or the miles driven without a passenger, can chip away at profits.
The service level also plays a big role. Ambulatory transport requires minimal equipment, while wheelchair transport needs specialized vehicles and modifications. Stretcher services demand even more - larger vehicles, pricier equipment, and often two staff members instead of one. Michelle McCullough, Marketing Manager at Broda, explains how specialized equipment can lead to significant cost savings:
NEMTs find they can replace as much as 90% of their stretcher trips and save an estimated $132,500 per year with two Traversa wheelchairs and a single operator per wheelchair.
Wait time is another cost factor. If drivers have to stay with patients during appointments, you're paying for their time without generating revenue. Many providers address this by charging wait-time fees in 15- to 30-minute increments.
Finally, time of service matters. Trips during weekends, holidays, or after-hours (typically after 5:00 PM) cost more because of higher driver wages. For example, holiday service rates are often 45% higher than those for regular weekday trips.
These trip-specific factors are essential in shaping your pricing model.
Standard U.S. Pricing Components
In the United States, most NEMT providers base their pricing on four main components:
- Base fee (load fee): Covers the initial pickup and varies by service level.
- Per-mile rate: Applies to the distance traveled with the passenger.
- Wait-time charges: Compensate drivers for time spent waiting during appointments.
- Surcharges: Cover special circumstances like no-shows, extra attendants, or specialized medical equipment such as oxygen.
Here's a typical breakdown of pricing by service type:
| Service Type | Base Rate (Weekday) | Base Rate (Weekend/Off-Hours) | Additional Mileage | Wait Time (per 30 min) |
|---|---|---|---|---|
| Ambulatory | $25–$30 | $30–$40 | $3–$5 per mile | $15–$30 |
| Wheelchair | $45–$50 | $75–$90 | $3–$5 per mile | $15–$30 |
| Stretcher | $100–$200 | $125–$225 | $3–$5 per mile | $15–$30 |
For example, a five-mile ambulatory trip during regular business hours typically costs around $21.18, while the same trip in a wheelchair vehicle averages $28.95. However, Medicaid reimbursement rates are often lower. In some states, wheelchair trips are reimbursed at $24.50, and ambulatory trips at $21.00 per trip.
These pricing elements form the foundation for deciding between flat-rate, mileage-based, or hybrid pricing models. As RouteGenie puts it:
If you charge too little, you won't make any money in NEMT. If you charge too much, potential customers will look to the more affordable competition.
Flat-Rate Pricing in NEMT
What Flat-Rate Pricing Is and When to Use It
Flat-rate pricing involves charging a fixed fee that covers the core tasks required for each trip. The fee depends on the level of assistance needed - whether the trip is for ambulatory, wheelchair, or stretcher-bound passengers. This pricing model works well for facility contracts with hospitals, dialysis centers, and nursing homes, especially when routes, distances, and trip schedules remain consistent. It's also a good fit for urban areas where shorter, more predictable distances make billing straightforward. As Michelle McCullough, Marketing Manager at Broda, explains:
For predictable routes you cover frequently, a flat rate is often the best model.
Benefits of Flat-Rate Pricing
Flat-rate pricing offers a clear and predictable structure, making it easier for customers to budget and plan. This approach has been linked to increased customer satisfaction - up by 20% as of March 2025. Additionally, flat rates help ensure that fixed costs, such as dispatching, vehicle prep, and loading time, are covered for every trip, even shorter ones, which helps protect your bottom line. The straightforward billing process also reduces administrative errors and speeds up reimbursements, especially when paired with NEMT-specific software.
Still, while flat-rate pricing has its advantages, it's not without challenges.
Drawbacks of Flat-Rate Pricing
One significant drawback of flat-rate pricing is the potential for undercharging on longer trips. If the flat rate is calculated based on average trip distances but passengers frequently require transportation over greater distances, the additional costs for fuel, driver time, and vehicle wear can quickly eat into profits. This makes the model less effective in rural areas where trip distances tend to vary widely.
Another challenge is the need to regularly review rates to stay competitive and ensure all operational costs are accounted for. As businesses grow, flat-rate pricing may struggle to keep up with rising expenses. RouteGenie highlights this point:
Every individual should determine their own pricing structure by analyzing their competitors, expenses, and aiming for the most profitable pricing while remaining competitive.
In contrast, mileage-based pricing can be a more flexible option for handling longer or less predictable routes.
Mileage-Based Pricing in NEMT
Mileage-based pricing offers a flexible alternative to flat-rate models, especially when trip distances vary significantly.
How Mileage-Based Pricing Works
This pricing model combines a flat pickup fee with a per-mile rate. For example, an ambulatory trip might begin with a base rate of $25–$30 during weekday business hours, adding $3–$5 per mile. Wheelchair trips typically have higher base rates, ranging from $45–$50, while stretcher transports start at $100–$200, often using the same per-mile charges.
Rates can be adjusted based on geography (rural areas often require higher per-mile rates), time (weekends, holidays, or off-hours), and unproductive "deadhead" miles to ensure cost recovery. Modern NEMT software simplifies the process by allowing you to tailor rate structures based on factors like vehicle type, time of day, and client needs. This adaptability ensures fair compensation while accommodating varying trip distances.
Benefits of Mileage-Based Pricing
One of the main advantages of mileage-based pricing is its ability to offer fair compensation for distance. This is especially important in rural areas where trip lengths can vary greatly. Unlike flat rates, which may leave you underpaid for longer trips, mileage-based pricing ensures revenue aligns with service demands.
From the client’s perspective, this model provides transparency. Breaking down costs into base rates and mileage charges on invoices helps customers see exactly what they’re paying for, fostering trust. For businesses, the model is also responsive to cost fluctuations. For instance, if fuel prices rise, you can adjust the per-mile rate without overhauling your entire pricing structure.
The benefits extend beyond individual trips. For example, Project TRIP, a rural NEMT program in Eastern North Carolina, charged $1.00 per mile for in-area trips and $0.75 per mile for out-of-area trips between January 2017 and December 2021. Over that period, they served 101 riders and saved $720,544 by reducing hospital admissions and emergency room visits. Additionally, the program showed health improvements, such as a 0.52 decrease in average A1C levels for users, highlighting the connection between transportation access and better chronic disease management.
Drawbacks of Mileage-Based Pricing
While mileage-based pricing has clear advantages, it also comes with challenges. One major issue is the administrative burden. Accurate documentation is critical, requiring GPS-verified trip data, patient or caregiver signatures, driver IDs, and mileage logs. As Mindbowser explains:
Medicaid demands proof. That means GPS stamps, patient or caregiver signatures, driver IDs, and mileage logs. No verification, no reimbursement.
Errors in manual data entry, such as odometer readings or HCPCS mileage codes, often lead to claim rejections. Studies show that up to 40% of NEMT billing staff hours are spent reworking denied claims, many of which stem from these errors. In fact, 10% to 20% of Medicaid NEMT claims are denied on the first submission due to documentation gaps or coding mistakes.
Fraud risks are another concern. For instance, discrepancies in mileage - like billing for 25 miles on a 12-mile trip - can trigger audits and denials. In one case, an Illinois NEMT provider faced $350,000 in clawbacks after an audit revealed gaps in GPS-verified trip data.
Another challenge is profitability for short trips. If the base fee is set too low, trips requiring significant hands-on service or extended time commitments may fail to generate sufficient revenue.
To address these challenges, consider implementing real-time GPS tracking to create accurate and defensible mileage logs. Automating eligibility verification through Medicaid API integration can streamline the process, and replacing paper logs with electronic signatures tied to GPS data can reduce errors and safeguard against audits.
sbb-itb-cef70f4
Flat-Rate vs. Mileage-Based Pricing: Side-by-Side Comparison
Deciding between flat-rate and mileage-based pricing boils down to understanding how each model aligns with your operations. Factors like market type, trip patterns, and administrative capacity play a big role in determining the best fit. Let’s break down the key differences to help you make an informed decision.
Profitability and Cost Coverage
Flat-rate pricing shines in predictable, short-distance routes, especially in urban areas. It ensures fixed costs are covered as long as trips stick to expected distances. However, it can become costly when delays or longer-than-anticipated trips occur.
Mileage-based pricing, on the other hand, adjusts revenue based on distance. This model accounts for rising fuel costs and vehicle wear but still requires a base fee to cover pickup costs. The way these models balance fixed and variable costs is critical to ensuring profitability in Non-Emergency Medical Transportation (NEMT).
Deadhead miles - those unpaid miles traveled to pick up passengers or return to base - can eat away 20% to 30% of profits. According to Elite Med Financials, the average NEMT vehicle runs at just 35% utilization. However, operators using AI-driven dispatch tools can increase that to 60%–80%, potentially adding $5,000 to $10,000 per vehicle annually.
| Feature | Flat-Rate Pricing | Mileage-Based Pricing |
|---|---|---|
| Fixed Cost Recovery | High for predictable short trips; risky for longer ones | Moderate; depends on base fee for pickups |
| Variable Cost Protection | Low; vulnerable to traffic and detours | High; adjusts with fuel and wear |
| Trip Length Variability | High risk for long trips | Low risk; revenue grows with distance |
| Service Level Differences | Managed with tiered flat fees (e.g., $50 for wheelchair, $30 for ambulatory) | Combines base rate with per-mile fees |
Ease of Use
Flat-rate pricing is simple and quick to quote. Clients receive an upfront, fixed price, making it easy to manage billing. Dispatch software can also be set up with fixed "zones" or "routes", which is particularly useful for consistent facility contracts.
Mileage-based pricing, while more precise, involves extra administrative work. Accurate mileage calculations are necessary for quotes and billing, often relying on GPS or odometer readings. Dynamic routing software becomes essential to ensure real-time accuracy.
| Feature | Flat-Rate Pricing | Mileage-Based Pricing |
|---|---|---|
| Quoting Speed | Instant; no calculations needed | Requires GPS or mapping tools |
| Billing Simplicity | High; easy for clients to understand | Moderate; detailed logs required |
| Software Integration | Simple; uses fixed data points | More complex; needs real-time tracking |
| Administrative Burden | Low; minimal documentation | Higher; requires accurate mileage records |
These operational differences make each model better suited for specific scenarios.
Best Fit by Market Type
Market type also plays a huge role in choosing the right pricing model. Each segment has unique demands that influence which approach works best.
Medicaid contracts often rely on hybrid models, combining a base rate with mileage fees. This structure aligns with how state programs and brokers handle reimbursements. For example, Medicaid reimbursement rates vary widely - New York pays $45–$120 for wheelchair trips, while Mississippi offers $16–$38.
Facility contracts with hospitals or nursing homes usually favor flat-rate pricing. These organizations value predictable monthly billing for frequent, short-distance trips, which simplifies budgeting and invoicing.
Private-pay clients benefit from hybrid or tiered models, allowing providers to charge premium rates for top-tier service while still covering distance-related costs. Margins for private-pay services can range from 20% to 30%, compared to Medicaid’s tighter 10% to 15% margins.
| Market Type | Preferred Model | Reasoning |
|---|---|---|
| Medicaid | Hybrid (Base + Mileage) | Matches state reimbursement structures |
| Facility Contracts | Flat-Rate | Predictable billing appeals to hospitals and nursing homes |
| Private-Pay | Hybrid or Tiered | Supports premium service fees and distance-based costs |
| Urban Markets | Flat-Rate | Dense routes make fixed pricing efficient |
| Rural Markets | Mileage-Based | Accounts for longer trips and higher fuel costs |
Each market type has distinct needs, making it important to tailor your pricing strategy accordingly.
Hybrid Pricing Models for NEMT
Hybrid pricing combines a flat base rate with mileage-based charges, offering a flexible way to cover fixed costs while adjusting for longer trips. This approach blends the strengths of flat-rate and mileage-based models, creating a balanced solution for trips of varying distances.
Common Hybrid Pricing Structures
The most widely used hybrid model is the base rate plus mileage structure. In this setup, you charge a flat "pickup fee" or "load fee" for every trip, then add a per-mile rate on top. For instance, you might charge a $45 base rate for wheelchair transport, with an additional $3 per mile traveled. The base rate accounts for the time and effort involved in loading the passenger, while the mileage fee covers fuel and vehicle wear.
Another variation is the base rate with mileage inclusion, where the base fee includes a specific number of miles - say, the first 5 or 10 miles - and additional mileage is charged only beyond that threshold. This model works particularly well in urban areas where trips are typically shorter, while still protecting against revenue loss on occasional long-distance journeys.
"A pickup fee with a standard mileage inclusion makes more sense, with a per-mile rate for longer trips (e.g., more than five or ten miles)." - Keren Dinkin, Content Strategist, NY BillPro
Tiered service rates add another layer of customization by setting different base fees depending on the level of care required - ambulatory, wheelchair, or stretcher - while maintaining a consistent per-mile rate across all service types. Some providers also incorporate radius-based charging, adding fees for "deadhead miles" when trips start or end outside a designated service area.
When Hybrid Pricing Makes Sense
Hybrid pricing shines in scenarios where neither flat-rate nor mileage-based pricing alone is sufficient. It’s particularly effective for services with varied trip distances, ensuring profitability on long trips while staying competitive for shorter ones. This flexibility is essential when serving a mix of facilities like hospitals, dialysis centers, and nursing homes, each with different distance needs.
Medicaid contracts often favor hybrid models because they align with state reimbursement structures that combine base rates and mileage fees. For private-pay clients, hybrid pricing allows for more dynamic and premium pricing options. If your business handles both Medicaid and private-pay clients, this model can help you navigate strict government rates while maintaining flexibility for private clients.
"This model [Base Rate Plus Mileage] is beneficial when the distance to different facilities varies greatly." - Michelle McCullough, Marketing Manager, Broda
However, managing hybrid pricing requires attention to detail. Investing in NEMT-specific billing software can simplify the process by automatically calculating base fees, mileage, wait times, and any additional equipment charges. Relying on manual calculations increases the risk of errors and claim rejections, so software can save time and reduce disputes, ensuring accuracy and efficiency in billing.
Conclusion: Selecting Your Pricing Model
The right pricing model for your business hinges on understanding your specific needs and circumstances. Start by evaluating your trip patterns. For urban routes with predictable, short distances, flat-rate pricing often makes the most sense. On the other hand, for rural areas or routes with varying distances, mileage-based pricing ensures you're covering costs effectively. Michelle McCullough from Broda sums it up well:
Profitability is a delicate balance between your costs, time, and choosing the best pricing structure.
Another key factor is your payer mix. Medicaid contracts generally come with fixed fee schedules, while private-pay clients allow for more pricing flexibility. If you serve both, a hybrid model - combining a base rate with mileage charges - can help balance profitability and accessibility.
Don't underestimate the role of technology in this equation. Manual pricing calculations can lead to billing errors and slow reimbursements. NEMT-specific billing software simplifies the process by automating pricing structures, tracking deadhead miles, and reducing claim rejections. These tools also make it easier to adapt your pricing strategy as market conditions change.
Regularly revisiting your pricing strategy is essential. Costs like fuel, insurance, and competition fluctuate, so reviewing your operational expenses every few months ensures your rates remain competitive and sustainable. Emmy Kolbe from RouteGenie highlights the stakes:
If you charge too little, you won't make any money in NEMT. If you charge too much, potential customers will look to the more affordable competition, instead.
Ultimately, whether you opt for flat-rate, mileage-based, or hybrid pricing, success lies in aligning your model with your market realities and staying flexible as your business evolves.
FAQs
How do I decide between flat-rate and mileage-based pricing for NEMT services?
Choosing between flat-rate and mileage-based pricing comes down to understanding a few crucial elements of your business. Start by looking at your fixed costs - things like vehicle leases, insurance, licensing, and driver wages. Then factor in variable costs such as fuel and maintenance, which naturally increase with trip distance. It’s also essential to think about the typical trip lengths and mileage patterns in your area, as well as any specialized services or equipment you offer, like wheelchair-accessible vehicles.
Don’t forget to examine your payer mix and reimbursement rates. These can play a big role in determining which pricing model aligns better with your financial goals. If you’re looking for simplicity and easier forecasting, a flat-rate model might be the way to go. But if your trips vary widely in distance, a mileage-based system could offer more precision. The best option will ultimately depend on how your business operates and what your customers need most.
What are the best ways for NEMT providers to simplify mileage-based pricing management?
To make mileage-based pricing easier, NEMT providers can rely on specialized dispatch and billing software. This type of software automatically tracks GPS mileage, calculates costs using a pre-set per-mile rate, and creates accurate invoices in real time. By automating these processes, you can avoid manual calculations, minimize errors, and speed up reimbursements - especially when dealing with Medicaid or third-party payers.
It’s also important to establish a clear fee structure that combines a base charge with a per-mile rate (for example, $50 plus $3 per mile). Embedding this pricing model into your software ensures consistency, makes billing straightforward, and helps you stay compliant with Medicaid and other regulations.
Lastly, connecting your billing system with accounting and claims platforms can automate data transfers, validate claims, and simplify payment workflows. These integrations not only make mileage-based pricing more efficient and transparent but also reduce the administrative workload.
What are the advantages of using a hybrid pricing model for NEMT services?
A hybrid pricing model, blending a flat rate with a mileage-based fee, gives NEMT providers more room to adapt and boost profitability. The flat rate covers fixed costs like vehicle upkeep, driver wages, and insurance, ensuring every trip starts on solid financial ground. The mileage-based fee, on the other hand, adjusts for variable expenses like fuel, vehicle wear, and driver time, making it a fairer system for longer journeys.
This pricing structure is straightforward to communicate. Medicaid payers appreciate the detailed cost breakdowns it provides, while private-pay clients value its predictability. It also allows providers to meet diverse market demands, offering competitive prices for short urban trips while maintaining profitability for longer rural routes. By balancing fixed and variable costs, the hybrid model promotes steady growth and minimizes the risk of underpricing extended trips.


